For millions of people with diabetes, the daily finger prick can be a painful and inconvenient reality when blood sugar levels need to be monitored Fortunately, technological advances have provided relief has emerged as diabetics without arteries, also known as continuous glucose monitoring (CGM) systems, provide readings, opening the door to a safer and more informed way of managing diabetes.
This comprehensive guide explores the world of painless diabetes measuring devices, evaluating the advantages, disadvantages, types, top competitors, and important factors to consider for making informed choices.
Why Ditch the Finger Prick?
Finger pricking, while effective, often presents challenges:
Pain:
Repeated pricking can be uncomfortable and discouraging, leading to skipped checks and inaccurate readings.
Convenience:
Carrying lancets, pricking devices, and test strips can be cumbersome and impractical.
Accuracy:
Fingertip glucose levels can fluctuate, leading to misleading readings, especially after meals or exercise.
CGMs address these issues by continuously measuring glucose levels with sensors worn under the skin. This sensor interfaces with the transmitter, sending real-time glucose data to a mobile app or receiver displayed on the device itself.
Benefits of Prickless Meters:
- Painless Monitoring: No more finger pricking means increased comfort and potentially improved adherence to monitoring schedules.
- Real-time Insights: Continuous glucose data provides a complete picture of glucose trends, not just snapshots, allowing for proactive diabetes management.
- Reduced Hypoglycemia Risk: Early warnings of glucose drops minimize the risk of hypoglycemic events.
- Improved A1C Levels: CGM use has been shown to improve glycemic control and A1C, a key indicator of long-term diabetes management.
- Enhanced Motivation: Seeing glucose trends in real-time can empower individuals to make informed lifestyle choices and stay motivated.
Drawbacks to Consider:
Cost:
CGM systems are generally more expensive than traditional meters, with ongoing sensor and transmitter costs.
Sensor Insertion:
While minimally invasive, some may find the sensor insertion process uncomfortable.
Accuracy Issues:
Sensors can sometimes produce inaccurate readings, requiring finger-prick calibration checks.
Technical Challenges:
CGM systems rely on technology, and malfunctions or connectivity issues can be frustrating.
Types of Prickless Meters:
Sensor-based CGMs:
These are the most common, where a sensor is worn under the skin, and the transmitter sends data to a client or app. Popular examples include the Dexcom G6, the FreeStyle Libre 2, and the Abbott Guardian Connect.
Interstitial Fluid (ISF) CGMs:
Glucose was measured by a sensor strip of interstitial fluid located immediately beneath the skin. Examples include Nutrisense CGM and Cygnos CGM.
Implantable CGMs:
These sensors are inserted under the skin and replaced every 3 months. Examples include Eversense CGM.
Top Contenders in the Prickless Arena:
Dexcom G6:

Known for its accuracy, real-time glucose trends, and smartphone compatibility, it requires calibration with finger pricks every 10 days.
FreeStyle Libre 2:
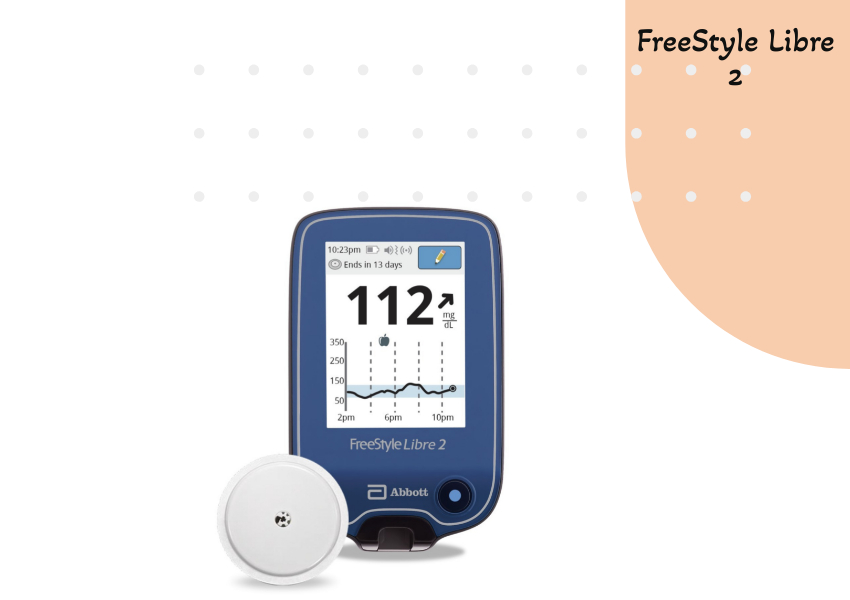
More affordable than the G6, it offers 14-day sensor wear and optional alarms for glucose highs and lows. However, real-time data requires a separate reader and doesn’t offer phone connectivity.
Abbott Guardian Connect:

This CGM boasts a rechargeable transmitter and 7-day sensor wear but requires calibration every 24 hours.
Choosing the Right Prickless Meter:
There’s no one-size-fits-all approach. Consider your needs, budget, lifestyle, and comfort level when selecting a CGM system. Key factors to ponder include:
- Cost: Consider both upfront device cost and ongoing sensor and transmitter expenses.
- Accuracy: Look for CGMs with proven accuracy and minimal calibration requirements.
- Features: Choose features that meet your needs, like alarms, trend graphs, and smartphone compatibility.
- Sensor Wear Time: Longer wear times mean fewer insertions and more convenience.
- Ease of Use: Opt for a system with user-friendly technology and readily available support.
Navigating the Priceless Future:
While forkless diabetes meters offer interesting possibilities, it’s important to consult with your healthcare provider before switching. They can help you determine if a CGM is right for you, recommend the best option for your needs, and guide you through the proper use and interpretation of glucose data.
Looking Beyond the Horizon:
The future of matchless diabetes management is exciting. Advances in sensor technology, machine learning algorithms, and data analytics promise more accurate and personalized glucose monitoring and pave the way
FAQs
Is a prickless meter right for me?
Discuss this with your healthcare provider. They can assess your needs and recommend the best option based on your diabetes type, lifestyle, and preferences.
How accurate are prickless meters?
While generally reliable, they can sometimes produce inaccurate readings. Finger-prick calibrations are often required to ensure accuracy.
What are the drawbacks of prickless meters?
Cost, sensor discomfort, and potential technical issues are some things to consider.
What are the differences between sensor-based, ISF, and implantable CGMs?
Sensor-based are most common, ISF use patches, and implantable are placed under the skin for longer wear. Discuss with your doctor which type might suit you best.
Does one CGM type offer more benefits than another?
Each type has its advantages and disadvantages. Sensor-based are widely available, ISF are less invasive, and implantable offer longer wear times. Consider your priorities when choosing.
What are the pros and cons of Dexcom G6, FreeStyle Libre 2, and Abbott Guardian Connect?
Each excels in different areas. Dexcom boasts accuracy and smartphone compatibility, Libre 2 offers affordability and 14-day wear, and Guardian Connect is rechargeable but requires frequent calibration. Explore their specifics to find your perfect match.
What features should I look for in a CGM?
Consider how important real-time trends, smartphone connectivity, alarms, sensor wear time, and ease of use are to you. Prioritize features that best suit your needs.
How much do prickless meters cost?
Expect to pay more than traditional meters, with ongoing sensor and transmitter expenses. Check if insurance covers CGM systems.
Are there ways to manage the cost?
Discuss financial assistance options with your healthcare provider and explore generic sensors or insurance rebates.
How do I use a CGM?
Instructions vary depending on the model. Your healthcare provider or the device manufacturer can guide you through the process.
How do I interpret the glucose data?
Learn how to identify patterns and trends in your readings. Your healthcare provider can help you understand what the data means for your diabetes management.
What do I do if I encounter technical issues?
Consult the device manual, contact customer support, or seek help from your healthcare provider.
How can a CGM help me manage my diabetes?
The continuous data can empower you to make informed lifestyle choices, adjust insulin doses, and prevent hypoglycemic events
How can I stay motivated with a CGM?
Utilize the data to set goals, track progress, and celebrate successes. Sharing your CGM data with your healthcare provider can also enhance support and motivation






